Cervicofacial subcutaneous emphysema is a rare complication of dental procedures with an air turbine or syringe, and dentists and oral surgeons sometimes encounter mediastinal emphysema following the presentation of extensive subcutaneous emphysema. Most emphysema occurs incidentally during tooth extraction, restorative treatment, or endodontic treatment, with only a few cases reported of cervicofacial subcutaneous emphysema associated with dental laser treatment. We report a case of cervicofacial subcutaneous and mediastinal emphysema caused by the air cooling spray of dental laser during dental treatment in a 76-year-old woman. After she underwent dental laser treatment, cervicofacial swelling was noted and she was referred to our department. Computed tomography showed both cervicofacial subcutaneous emphysema and mediastinal emphysema. Antibiotics were administered prophylactically and the emphysema disappeared 5 days after the dental laser treatment, without any complications.
Cervicofacial subcutaneous emphysema is a rare com- plication of dental procedures with an air turbine 1-3 or syringe, 1,4,5 and dentists and oral surgeons sometimes encounter mediastinal emphysema following the pre- sentation of extensive subcutaneous emphysema. 2-4 Most cases of emphysema occur incidentally during tooth extraction, 1-3 restorative treatment, 1 or endodon- tic treatment. 1,6 However, only a few reports have described cervicofacial subcutaneous emphysema asso- ciated with dental laser treatment. 7-9 We report here a case of cervicofacial subcutaneous and mediastinal em- physema caused by air cooling spray of dental laser during dental treatment.
CASEREPORT
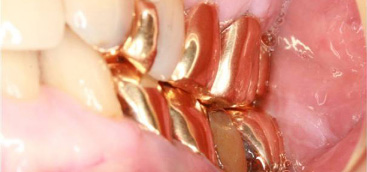
A 76-year-old woman presented to a family dental clinic with left upper gingival swelling and pain. Dental examina- tion revealed acute periodontitis of the left upper first molar. Under local anesthesia, the patient underwent calculus re- moval and Er:YAG laser irradiation to the gingival pocket. Immediately after the dental laser treatment, she felt discom- fort in the left cheek and subsequently developed bilateral cervicofacial swelling. As a result, the patient was referred by her dentist to our department with bilateral cervicofacial swelling ( Figure 1 ). Vital signs were normal, and oxygen saturation was 97% on room air. Although physical examination revealed diffuse swelling with crepitus from the bilateral temporal region to the supraclavicular fossa, no Hamman sign, dyspnea, or dys- phagia were present. Intraoral examination showed swelling of the buccal gingiva of the left upper first molar and the buccal mucosa ( Figure 2 ). We diagnosed this clinically as cervicofacial subcutaneous emphysema caused by air cooling spray of dental laser. Computed tomography (CT) of the thoracocervicofacial region revealed widespread emphysema from the cervicofacial space, including the buccal, masticator, submandibular, parapharyngeal, and retropharyngeal spaces, to the mediastinum and precordium ( Figure 3 ). We admitted the patient for airway monitoring, bed rest, and prophylactic intravenous antibiotic therapy. The cervicofacial swelling dis- appeared and the subcutaneous crepitus was almost undetect- able 5 days after the dental laser treatment. The patient was then discharged without any complications. Two weeks after the dental laser irradiation, CT showed no cervicofacial sub- cutaneous or mediastinal emphysema.
DISCUSSION Cervicofacial subcutaneous emphysema is an uncom- mon complication caused by dental treatment and oral surgery. 2,3,7-9 Subcutaneous emphysema is typically in-duced by tooth extraction, 1-3 but it can also occur as a result of various dental treatments, such as restoration and endodontic treatment. 1,6 Heyman and Babayof 10 reviewed 75 cases reported from 1960 to 1993 of sub- cutaneous emphysema and pneumomediastinum after dental treatment. Emphysematous complications were caused by the use of only a high-speed handpiece in 27 cases (36%) and with the use of both a high-speed handpiece and air syringes in 42 patients (56%). On the other hand, a review by McKenzie and Rosenberg, 1 covering cases reported from 1993 to 2008, showed that 16 of 32 cases (50%) of iatrogenic subcutaneous emphysema were linked to the use of air-driven hand- pieces. Arai et al. 2 also reviewed 47 CT-documented cases reported from 1994 to 2008 of subcutaneous emphysema and peumomediastinum following dental treatment and found the cause was use of a high-speed air turbine handpiece in 31 patients (66%). According to these reviews, the incidence of emphysema caused by high-speed air-driven handpieces during surgical or nonsurgical dental procedures has increased. 1,2,10 Because subcutaneous and mediastinal emphysema can occur during nonsurgical dental procedures, such as restorations and extractions, this suggests that air from the air turbine may enter the tissue even via a minor break in the mucosa. 2 In addition, rare cases have been reported following nonsurgical procedures where an air.
syringe was used to dry the oral mucosa. 4,5 The air entry points in these cases were a 4-mm superficial laceration of the buccal mucosa 4 and a 2-3-mm deep gingival pocket. 5 Furthermore, Kim et al. 6 reported subcutaneous emphysema and pneumomediastinum af- ter use of an air turbine and syringe in endodontic retreatment involving an airstream projected into the gingival sulcus. In our patient, compressed air associ- ated with use of the Er:YAG laser similarly entered the subcutaneous tissue via the gingival pocket. Lasers are now being used more widely in dentistry and oral surgery. 11,12 Dental laser therapy has been approved by the U.S. Food and Drug Administration for a number of dental and surgical soft-tissue proce- dures, including hemostasis, tumor removal, gingivoen- tomy, aphthous ulcer treatment, removal of canal filling material, gingival sulcular debridement, and abscess incision and drainage. 11 In Japan, dental laser therapy is now widely performed by dentists and oral surgeons using either an Nd:YAG, CO 2 , or Er:YAG laser. Nd: YAG and CO 2 lasers, which are commonly used high- power lasers, show excellent soft tissue ablation capa- bility and adequate hemostasis. 13 The effectiveness of Er:YAG lasers in periodontal treatment has been pre- viously reported. 13-16 Aoki et al. 13 showed that it is more effective than ultrasonic scaling of subgingival calculi, and Ando et al. 16 reported that the Er:YAG laser has a high bactericidal potential. The Er:YAG laser has recently been approved by the Ministry of Health, Labor, and Welfare in Japan for caries removal, cavity preparation, gingival sulcular debridement, and subgingival calculus removal. As a result, dental laser treatment is commonly performed in many dental clin- ics.
Emphysema as a complication caused by the air cooling spray of dental laser during dental procedures and oral surgery is not well known, although dental laser produces compressed air just as air turbine and syringe. Inaccurate use of dental laser with air projec- tion system can cause subcutaneous emphysema. 7,8 To our knowledge, there are only 3 case reports describing emphysema caused by the air cooling spray of dental laser. 7-9 In 2000, Hata and Hosoda 7 reported cervico- facial emphysema caused by CO 2 laser therapy for a gingival abscess, where the slender tip of the CO 2 laser, which had an air stream of 152 kPa directed toward the tip, was inserted, for 3 minutes, into the submucosal tissue above the root apex to cauterize an apical lesion. Imai et al. 8 also reported subcutaneous emphysema and pneumomediastinum after intraoral CO 2 laser irradia- tion of a periapical lesion. Air would have been directly introduced under the periosteum because of the close proximity of the laser tip to the abscess cavity during irradiation. In the third report, Matsuzawa et al. 9 doc- umented cervicofacial subcutaneous and mediastinal emphysema resulting from incision with a YAG laser for drainage of a gingival abscess due to periodontitis. In the present case, cervicofacial subcutaneous and mediastinal emphysema were caused by air cooling spray during Er:YAG laser irradiation to the gingival pocket. Considering all of these cases, mediastinal em- physema has occurred in 3 of 4 patients with cervico- facial subcutaneous emphysema associated with dental laser irradiation. Although the air pressure of a dental laser is lower than that of an air turbine, the length of time that the tip is inserted might be related to the risk of emphysema. 9 According to a dental laser manual, the method of incision is first to cut the part of the swollen gum for opening with the laser and to secure drainage. 9 In addition, the laser should be used without fixing the tip in the same location in submucosal tissue while advancing and retracting it. 9 The Er:YAG laser manual suggested that the air pressure toward the laser tip should be lowered or turned off when irradiating a gingival sulcus. However, even if the air pressure were turned off, moderate air flows continue toward the tip for cooling and protection. Prevention of laser-induced emphysema in accessing a closed or narrow cavity, such as a submucosal abscess or surgical defect, requires careful adjustment of the assist airflow and the avoidance of focused and pro- longed laser irradiation. 8 It is extremely important to recognize the potential risk of iatrogenic emphysema caused by the air cooling spray of dental laser during dental treatment and oral surgery. Dentists and oral surgeons should stop any procedures when patients report discomfort or complain of swelling or pain. In such cases, the dentist or surgeon should arrange for a CT scan from the face to the chest to identify the extent of emphysema and administer antibiotics prophylacti- cally to avoid infection.

